It’s understandable why anesthesia-free dental cleanings sound reassuring. Many people worry about the risks of anesthesia, especially for older pets or pets with underlying health conditions, and the idea of a “safer” or less invasive alternative can feel comforting. But much of dental disease happens below the gumline, where painful infection, inflammation, and tissue damage cannot be seen or treated while a pet is awake. An anesthesia-free cleaning may remove visible tartar from the surface of the teeth, but it cannot provide the comprehensive examination, dental X-rays, cleaning beneath the gums, or safe treatment that true veterinary dentistry requires. In many cases, these procedures create the appearance of a healthy mouth while painful disease continues to progress unnoticed. As a specialty veterinary dental practice, we believe you deserve clear, honest information about what anesthesia-free dental cleanings can and cannot accomplish, and why properly monitored anesthesia is often the safer choice for meaningful dental care.
North Bay Veterinary Dentistry in Petaluma is a specialty referral practice focused entirely on veterinary oral health. Dr. Fulton and our team perform thorough dental procedures under proper anesthesia protocols with careful monitoring, which is how we deliver care that makes a genuine clinical difference, not just cleaner-looking teeth. Contact us to learn more or request a referral.
Are Anesthesia-Free Dental Cleanings Illegal in California?
In some cases, yes. California law states that anyone who uses a tool to scrape tartar off of the teeth of a pet must be under the direct supervision of a veterinarian. That means that anesthesia-free dentals (AFDs) offered by groomers, human dental technicians or dentists, or literally anyone else without a veterinarian in the room are operating illegally.
Why was this made illegal? Because the medical risks and behavioral consequences are real. Tooth brushing is a different story- groomers and other non-veterinary staff are allowed to brush your pet’s teeth.
What Can Anesthesia-Free Cleanings Actually Do?
The visible portion of a tooth, the crown, is where anesthesia-free cleaning concentrates its effort. A practitioner uses hand scaling tools to scrape tartar off the front, accessible surfaces of the teeth. The patient is restrained, sometimes wrapped in a towel, while the procedure is performed.
This produces a visually cleaner mouth. The tartar that was visible on the front of the teeth is gone, and from the outside, the cleaning appears to have worked.
What it cannot do is what actually matters most:
- Cannot clean below the gumline, where periodontal disease lives
- Cannot clean the inner surfaces of teeth
- Cannot reach the back molars in a struggling, awake animal
- Cannot perform dental radiographs, which are essential for identifying disease invisible to the eye
- Cannot diagnose tooth root abscesses, resorptive lesions, or jaw bone disease
- Cannot extract painful diseased teeth
The conclusion is direct: anesthesia-free cleanings provide cosmetic benefit while leaving the clinically significant disease entirely unaddressed. Multiple studies performed comparing pets who received AFDs with dogs who received no care and dogs who received professional cleanings under anesthesia showed that dogs with AFDs had no actual improvement in their oral health. In some cases, their oral health was worse.
The Welfare Concerns of Restrained Awake Procedures
Beyond the clinical limitations, there are legitimate welfare concerns about anesthesia-free cleanings.
A pet undergoing anesthesia-free dental work is restrained, often forcibly, while sharp instruments are used in their mouth. They cannot consent, cannot understand what’s happening, and often experience the procedure as a frightening, prolonged traumatic event.
Risks during restrained awake procedures include:
- Soft tissue lacerations: from sudden movements against sharp instruments
- Dental fractures: from inappropriate pressure on already-compromised teeth
- Aspiration of debris: the unprotected airway can lead to aspiration pneumonia
- Stress-related cardiac events: especially concerning in pets with underlying heart disease
- Long-term behavioral consequences: fear of mouth handling that interferes with future care
- Inadequate cleaning: disease left untreated despite the appearance of effort
Anyone who has tried to brush their pet’s teeth knows how hard it can be to get them to sit still for even 30 seconds, and that’s with a plastic, soft-bristle brush. Now imagine that for 30 to 60 minutes with razor-sharp tools and a stranger instead.
Are Pets Who Received Anesthesia-Free Dentals More Likely to Need Specialty Care?
Often, yes. Picture this:
Dog #1 receives brushing and dental chews at home every day. They had their first professional anesthetized cleaning at age 3, and then one every year and a half or so with their regular veterinarian. By the time they are 10, their dental disease is minimal; the home care prevented problems from the start, the X-rays caught problems early, and the regular deep cleanings stopped disease before it was severe. No specialist needed.
Dog #2 also receives brushing and dental chews. They had their first AFD at the age of three, then one every year and a half or so at the local groomer. They didn’t like being restrained, so the groomer could never reach the molars, and no cleaning under the gumline or X-rays were ever taken. The bottoms of their teeth look clean, but disease lurks under the surface. By the time they are 10, their dental disease has progressed to the point where they need 10 or more teeth removed and their jaw bone is so weakened that they fractured it just from chewing on their favorite toy. Now you’re looking at thousands of dollars in advanced specialty dental work on top of the pain and damage to the heart, liver, and kidneys from constant infection and inflammation.
Two similar dogs, two very different stories.
Why Is Modern Veterinary Anesthesia Safer Than Most People Realize?
The fear of anesthesia is reasonable. It’s also typically based on outdated information. Modern veterinary anesthesia and dental cleaning protocols include the same medications, precautions, and monitoring that human hospitals use:
- Pre-anesthetic exam: identifies concerns before the procedure begins
- Pre-anesthetic bloodwork: confirms organ function and uncovers hidden risks
- Individualized protocols: matched to the specific pet’s age, health, and medications
- Intubation: protects the airway throughout the procedure and prevents aspiration
- Continuous monitoring: heart rate, oxygen saturation, blood pressure, ECG, body temperature, and end-tidal CO2
- IV catheter: provides fluid support and a route for rapid intervention if needed
- Trained anesthesia personnel: dedicated to monitoring throughout the procedure
- Tailored recovery support: warming, pain management, and close observation
For patients at North Bay Veterinary Dentistry, we also offer consultation with a board-certified veterinary anesthesiologist and team members who have worked directly with anesthesiologists. The risk of complications from a properly performed dental anesthesia in a healthy pet is genuinely small. The risk of leaving advanced periodontal disease untreated is genuinely substantial.
Are Dental X-Rays Really Necessary For Pets?
Dental X-rays are not optional in proper veterinary dentistry.
Consider how often your own dentist recommends X-rays, and that’s with you brushing twice daily, flossing, and getting a full cleaning at least once a year, preferably twice.
Now consider your pet. They chew on sticks, rocks, bones, your furniture, and anything else they can find. They eat poop, collide full-speed with other dogs at the park, play tug using their teeth instead of hands, and rely on you to have their teeth brushed. Their dental damage accelerates quickly, with most pets having disease by the age of three.
What dental radiographs commonly reveal that examination alone cannot:
- Tooth root abscesses developing under apparently normal-looking teeth
- Resorptive lesions in cats (a painful condition where the tooth structure is being broken down by the body itself)
- Retained tooth roots from previous extractions
- Jaw fractures including pathologic fractures from advanced periodontal disease
- Bone loss that’s invisible above the gumline
- Cysts and tumors developing in the jawbone
Our digital imaging capabilities include full-mouth dental radiography and Cone Beam CT for three-dimensional skull imaging. This level of imaging dramatically reduces both anesthesia time and the diagnostic uncertainty that produces incomplete treatment.
A cleaning without imaging, anesthesia-free or otherwise, cannot diagnose the conditions that most warrant treatment. Your pet leaves the procedure with the same disease they arrived with, just less visible tartar.
What Comprehensive Veterinary Dentistry Actually Includes
Pet dental care at a specialty level extends well beyond cleaning. Anesthesia allows us to provide advanced treatments while your pet is safely and comfortably asleep.
Periodontics
Periodontal therapy addresses the most common dental disease through several techniques:
- Subgingival scaling and root planing to remove tartar and smooth root surfaces
- Perioceutics (placement of antibiotic gels into pockets)
- Periodontal flap surgery to access deep pocket disease
- Guided tissue regeneration with bone graft material to restore lost support
- Selective extraction of teeth that cannot be saved
These procedures cannot be approximated by an awake cleaning at any level.
Endodontics
Root canal therapy saves teeth that would otherwise require extraction. Common indications include fractured teeth with pulp exposure, dead teeth from blunt trauma, and teeth with deep cavities affecting the pulp. The procedure preserves the structural integrity of the tooth while eliminating the source of pain and infection.
Orthodontics
Orthodontic treatment corrects malocclusions (incorrect bite alignment) that cause pain, oral trauma, or interference with normal eating. Common interventions include treatment of base-narrow lower canines, overbites, and underbites.
Prosthodontics
Crown or cap placement protects compromised teeth in specific situations: police and working dogs with fractured canines, teeth with subgingival fractures that have been root-canal treated, and certain wear patterns that threaten tooth integrity. Metal alloy crowns provide durable protection for teeth where preservation matters.
Oral Surgery
Oral surgery addresses fractured teeth, oral tumors, oronasal fistulas, retrobulbar abscesses, and mandibular fractures among other major surgical needs. These conditions require surgical expertise that no awake procedure can address.
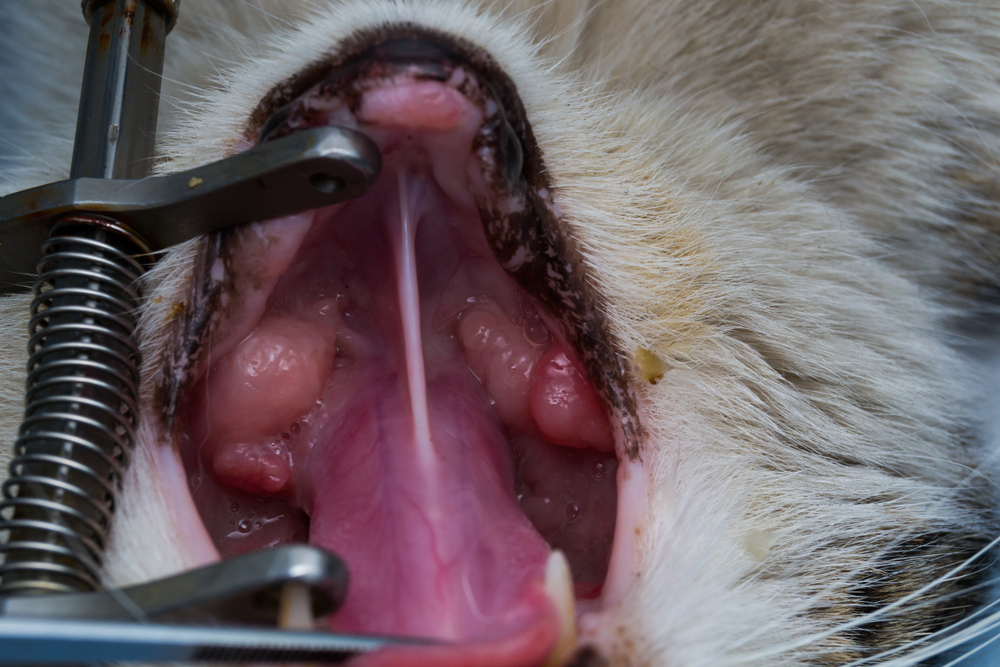
Stomatitis Treatment
Feline chronic gingivostomatitis (FCGS) and Canine plaque-reactive stomatitis (CUPS) are severe inflammatory diseases of the mouth that produce extreme pain. Treatment of FCGS typically involves extraction of premolar and molar teeth, achieving cure in approximately 60 percent of cases and significant improvement in another 20 percent. Refractory cases may require steroids, immunosuppressants, or stem cell therapy. CUPS requires regular anesthetized cleanings, daily brushing, and selective extractions for management. Without anesthesia, these pets live in constant pain.
What Does Effective Home Dental Care Actually Look Like?
Daily home care is the foundation that extends the benefit of professional cleanings. The combination matters more than either alone.
For products with documented effectiveness, look for the VOHC seal (Veterinary Oral Health Council). Products carrying the seal have demonstrated measurable plaque or tartar reduction in clinical trials. Without the seal, marketing claims should be viewed skeptically.
Effective home care strategies include:
- Daily brushing with pet-specific enzymatic toothpaste (never human toothpaste; xylitol and fluoride are toxic)
- Dental wipes or gauze as alternatives for pets who won’t accept a brush
- VOHC-accepted dental chews sized appropriately to the pet
- Water additives as supplemental support
- Prescription dental diets for pets with significant tartar predisposition
- Avoiding hard chews (antlers, hooves, hard nylon, real bones) that fracture teeth
Even the most committed home care cannot substitute for professional cleanings, but it dramatically extends the interval between procedures and prevents the deepest disease from establishing.
Frequently Asked Questions About Anesthesia-Free Dentistry
My friend’s dog had an anesthesia-free cleaning and seemed fine. Why is it a problem?
Many pets tolerate the experience and visibly leave with cleaner-looking teeth. The problem usually isn’t the immediate experience; it’s what’s left untreated. The disease the procedure couldn’t address continues to progress, often becoming more advanced before the next attempt at care. By the time the limitations become evident, treatment is more invasive and more expensive.
Isn’t anesthesia dangerous for older pets?
Modern anesthesia for healthy senior pets is generally very safe with proper protocols, monitoring, and pre-anesthetic evaluation. For pets with significant chronic disease, individualized protocols and consultation with a board-certified anesthesiologist make procedures safe in most cases. The decision should be based on your specific pet’s situation, not a blanket fear of anesthesia.
Is there ever a role for AFD cleaning between professional procedures?
Daily home care like brushing is the appropriate “between cleanings” maintenance. Some pets benefit from supplemental care like dental wipes or treats. What doesn’t fit in this role is restrained awake “cleaning” that creates the appearance of professional care without its substance.
Honest Care for Your Pet’s Mouth
The reason anesthesia-free dental cleaning has gained traction isn’t because it’s clinically effective. It’s because it appeals to real concerns about anesthesia, cost, and convenience. We understand those concerns. We also believe that addressing them with a procedure that doesn’t actually treat dental disease isn’t the right answer.
When your pet needs dental care, they deserve care that genuinely addresses what’s wrong. Our team, led by Dr. Fulton, is built for that work. We provide individualized anesthesia protocols, comprehensive imaging, and the full range of dental services that proper anesthesia enables.
If your veterinarian has recommended a dental specialty referral, request an appointment for new patients or use our existing client appointment request for established patients. We’d be glad to evaluate your pet’s mouth and explain what their care requires, honestly and thoroughly.



Leave A Comment